“In one ear and out the other.”
“Doesn’t listen to a word I say. He just zones out.”
When parents describe their children like this, I think about potential working memory problems.
Increasingly, Google-savvy parents ask for my views on whether their language-delayed child might benefit from an expensive working memory training program to help their language development. So what do I tell them?
First, some basics:
1. Working memory as a mental jotting pad
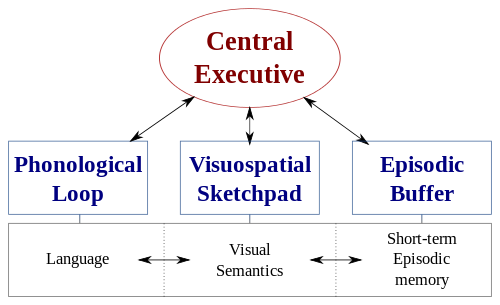
There are several technical definitions of working memory. Probably the most well-known model comes from Baddeley (2000):
For our purposes, we can (conveniently!) side-step an explanation of each of the components of this model and simply define working memory as a mental system that provides a kind of mental jotting pad storing information for things like following directions and remembering numbers (Gathercole, 2008). It’s a “bottom level” processing skill (in contrast to language, which is a “top level” collection of skills).
2. What does a working memory problem look like?
About 10% of children have a clinically impaired working memory. In the classroom, the typical profile of these children looks like this:
- normal social relationships with peers;
- quiet and reserved in group work;
- difficulties with reading and maths;
- difficulties following instructions; and
- may appear to be inattentive, to have a short attention span or to be distractable.
Confusingly, some aspects of this profile are also seen in children with language disorders and/or auditory processing disorder and/or ADHD. Sometimes, the child needs to be seen by a speech pathologist, audiologist and mental health professional to figure out what’s going on. Many children with language disorders have working memory problems (see below). Most children with working memory problems don’t tend to be hyperactive or impulsive, although the majority of children with ADHD have working memory problems (Holmes et al, 2008).
3. Why do many children with working memory problems struggle at school
Gathercole and Alloway (2008) think it’s because these children can’t meet the memory demands of structured learning activities. Their working memory “becomes overloaded and the crucial information that is needed…such as the sentence they are attempting to write, or the sequence of instructions they need to follow is lost.” The child is forced to either guess or abandon the task.
4. Why do some of these children zone out?
According to Gathercole and Alloway’s theory, “zoning out” occurs when working memory is so overloaded that it is no longer possible for the child to keep in mind the information needed to stick with the activity. As the child loses the information needed to guide the activity they are working on, their attention shifts away from what they are doing.
5. Why is everyone suddenly talking about working memory training programs?
In recent years, several working memory intervention programs have been developed, some commercially. These include:
- so-called “dual n-back” tasks based on the research of Dr Jaegii and colleagues (2008); and
- CogMed, a computer-based working memory program owned by Pearson that is designed to “stimulate cognitive change, especially working memory and attention”. Many health professionals (including speech pathologists) are training to become accredited as CogMed “coaches” licensed to deliver the program to their clients.
The attraction of programs like these to families is understandable. Learning to use language effectively is hard for anyone, but especially for children with language and learning disorders. Sometimes, language and reading problems seem almost insurmountable. Interventions that target underlying processing skills, like auditory processing and working memory can be attractive to families because the treatments seem to suggest that complex skills like language can be improved by targeting underlying skills, rather than the advanced skills and knowledge needed to be a good speaker, listener, reader and writer (Kamhi, 2014).
It’s a lovely thought. But is it supported by evidence?
6. Working memory and language disorders
As the Greeks knew, memory and language are related. There’s a large body of recent evidence showing children with language and learning disorders typically perform below norms on measures of phonological short-term and working memory, suggesting that working memory problems contribute to language disorders, at least for some children (e.g. Boudreau & Costanza-Smith, 2011; Leonard et al., 2007). This has led many researchers to ask an important question:
If working memory is an underlying cause of some language and learning problems, will improvements in working memory lead to significant changes in language function?
So far – unfortunately – the answer appears to be “no“.
A 2013 meta-analysis by Melby-Lervag & Holme of 23 working memory studies found no evidence that memory training was an effective intervention for children with dyslexia or ADHD. Working memory training did not lead to better performance outside the specific memory tasks trained. The researchers concluded that their findings “cast strong doubt on claims that working memory training is effective in improving cognitive ability and scholastic achievement”. In other words, children in these studies improved their working memories on the tasks they practiced, but these gains did not seem to transfer to real world improvements in language or reading.
7. So what can we do to help children with working memory problems cope with school?
Gathercole suggests:
- being alert for the signs, especially incomplete recall, failure to follow instructions and giving up on tasks;
- monitoring the child, watching for warning signs;
- reducing working memory loads: shortening sentences, providing visual and other context, breaking complex tasks into simple tasks and multistep instructions into one-step instructions;
- repeating important information;
- using memory aids, e.g. wall charts, posters, personal dictionaries, counters, abacuses, calculators, memory cards, audio recorders and computer software; and
- helping children find and use their own strategies, e.g. asking for help, rehearsal, note-taking, use of long-term memory, placekeeping and organisational strategies
8. Clinical bottom line: what I tell client families
In light of the current evidence base, for children with a profile suggesting working memory issues:
- I assess working memory as part of my assessment battery; and
- if working memory is an issue, I recommend teachers employ the kinds of classroom strategies suggested by Gathercole and colleagues (see part 7 above); and
- I do not currently recommend working memory training programs to treat language disorders.
However, as with auditory processing disorder, we all need to keep an open mind on this developing area of practice. Important research continues on working memory interventions, including investigations into ways of improving the transfer of working memory gains to higher level functions, like language and reading.
For specific working memory programs, such as CogMed, I tell my clients to look at independent reviews by experts.
I find aspects of CogMed and other working memory interventions theoretically very promising; and I would love to see some quality, independent research to support the use of working memory programs to improve language skills. In the meantime, however, I will continue to take a “top down” approach, working to improve my clients’ language skills by working on language goals, and to improve my clients’ reading skills by working to improve reading, decoding and comprehension skills.
Principal sources: Gathercole, S.E. (2008). Working Memory in the Classroom. The Psychologist, 21(5), 382-385. Diamond, A. & Lee, K. (2011). Interventions Shown to Aid Executive Function Development in Children 4 to 12 Years Old. Science 333, 959 and Kahmi, A.G. (2014). Improving Clinical Practices for Children with Language Disorders. Language, Speech, and Hearing Services in Schools, 45, 92-103. Picture of Baddeley model from here.
Image: http://bit.ly/1IB5uu2

Hi there, I’m David Kinnane.
Principal Speech Pathologist, Banter Speech & Language
Our talented team of certified practising speech pathologists provide unhurried, personalised and evidence-based speech pathology care to children and adults in the Inner West of Sydney and beyond, both in our clinic and via telehealth.



Leave a Reply